
The Rise of Workplace Opioid Abuse

Written by: Virginia McCormick, NES, Inc.

Employers are increasingly finding themselves confronting the realities of workplace opioid abuse.
Opioid Abuse an Enduring Concern in the Nation
The odds of dying accidentally from an opioid overdose rose in 2018 to one in 96, according to an analysis published by Injury Facts, an extension of the National Safety Council (NSC). For the first time in U.S. history, it is now more likely that a person will die from an accidental opioid overdose than from a motor vehicle crash (one in 103). More than 100 people die from an opioid overdose every day – 37,814 people every year.
Opioid use in the U.S. has been rapidly increasing in the last decade, with 66.4% of the 63,632 drug overdoses in 2016 involving opioid abuse. According to the Centers for Disease Control and Prevention (CDC), that figure rose in 2017 to around 68% out of 70,200.
Alongside the nation’s overarching crisis, opioid abuse in the workplace has steadily risen in recent years. According to the Bureau of Labor Statistics, reported overdose deaths at work from the non-medical use of drugs increased by 38% between 2013 and 2016.
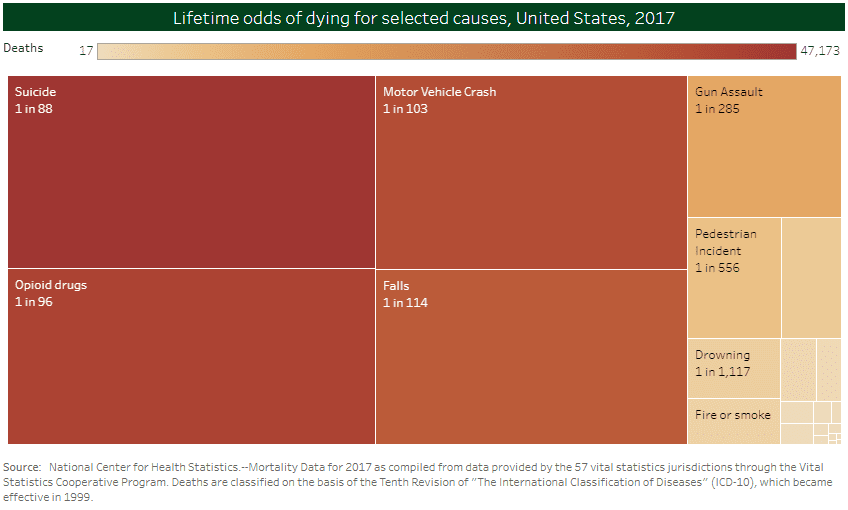
It is now more likely to die from an accidental opioid overdose than from a motor vehicle crash. Source: Injury Facts
While this increase includes all non-medical drug use and not just workplace opioid abuse, it does parallel an overall increase in overdose deaths from opioids reported by the CDC. Additionally, according to a March 2019 NSC survey, 75% of employers stated that their workplaces had been directly impacted by opioid use.
The existence of workplace opioid abuse is understandably difficult to confront, but experts like Nick Smith, CEO of NSC, assert that meaningful change can only occur once we acknowledge this reality.
“… The No. 1 cause of preventable death is not just taking its toll on our home lives, but companies across the country are also grappling with the impact of this epidemic,” said Smith. “If there is a silver lining, it’s that we have an opportunity to gain the attention and resources of American businesses to combat this societal scourge.”
Opioid Crisis Synopsis
Primarily used for pain relief, opioids are commonly divided into three categories: natural opioids, semi-synthetic opioids, and fully synthetic opioids. Opioids, according to the NIH, include “heroin, synthetic opioids such as fentanyl, and pain relievers available legally by prescription, such as oxycodone (OxyContin®), hydrocodone (Vicodin®), codeine, morphine, and many others.”
Most forms of opioids are controlled substances due to their addictive properties and potential to cause respiratory depression and death in high doses.
The U.S. opioid crisis, as it is now commonly referred to, began with increased prescriptions in the late 1990s. According to the National Institute on Drug Abuse (NIH), pharmaceutical companies assured patients they would not become addicted to opioid pain relievers, and consequently healthcare providers began to prescribe them at greater rates. By the time it became clear that prescribed opioids were habit-forming and potentially dangerous, overdose rates had begun to increase dramatically.
As reported in NIH opioid crisis data, 21 to 29% of patients who were prescribed opioids for chronic pain have misused them, 8 to 12% developed an opioid use disorder, and opioid overdoses increased 30% in 45 states from July 2016 to September 2017.
The primary way to prevent opioid overdose death is by administering the medication naloxone. Naloxone, best known commercially as Narcan®, is an “opioid antagonist” used to treat overdoses by effectively blocking the opioid receptors in the brain. It is publicized as being able to, “completely reverse the effects of an opioid overdose if administered in time” by restoring normal respiration.
For more information on naloxone, see our July 2017 blog post, Increased Access to Naloxone is Saving Lives, which covers the life-saving medication in greater depth.
If an opioid or other drug overdose is suspected in the workplace, responders should immediately contact emergency services via 9-1-1, even if naloxone is administered. Medical assistance is always necessary in the event of a suspected overdose. For more information, see the National Institute for Occupational Safety and Health (NIOSH) flyer Responding to a Suspected Opioid Overdose.
Opioid overdoses increased 30% in 45 states from July 2016 to September 2017, according to NIH.
Implications of Workplace Opioid Abuse
A wide variety of workplace injuries, such as those resulting from slips, trips, and falls or from lifting heavy loads, may require a pain reliever to be prescribed. Workplace hazards therefore have the potential to be associated with prescription opioid use – and abuse.
Additionally, employees such as first responders, law enforcement personnel, and hospital workers who are in regular contact with high-risk environments and/or high-risk individuals are reported as more likely to abuse opioids themselves. Other risk factors include genetics, familial substance abuse, and economic status.
Workplace opioid abuse is a major concern for employers around the country, as health care costs for employees who abuse prescription drugs are reportedly three times higher than those for an average employee. NIOSH research shows that employees with a current substance abuse disorder miss about 15 workdays per year, and a subset of those with a pain medication use disorder miss about 29 days per year. This contrasts with an average of 10 missed days per year for most employees.
In a March 2019 NSC survey, 41% of employers stated that they, “would return an employee to work after he or she receives treatment for misusing prescription opioids.” However, the same survey showed that only 17% of employers felt extremely well prepared to deal with the issue, despite most of those same responders starting that their workplaces had been impacted by opioid use.

Workplace opioid abuse may lead to increased employee health care costs and missed workdays.
Workplace Opioid Abuse: How Employers Can Help
One of the biggest challenges in the fight against opioid abuse is a misunderstanding of who the drug affects. Opioids, when not being abused, are considered by many to be an invaluable method of pain management and comfort to those who are suffering from an injury or illness.
But even short-term opioid use can lead to addiction. This, coupled with pressure not to miss work or slow down their co-workers, can be a recipe for disaster. It is important for employers and their employees to recognize that the multi-faceted realities of workplace opioid abuse can be damaging for everyone involved. And according to the NSC, “employer supported and monitored treatment yields better sustained recovery rates than treatment initiated at the request of friends and family members.”
The NSC recommends employers implement and follow these drug-free workplace practices to help prevent workplace opioid abuse and keep employees safe:
- Develop a clear, written policy (often developed in tandem with legal counsel) regarding drug use prevention, risk management, and liability at the workplace
- Provide employee education on prescription needs, seeking addiction or dependency help, and possible effects opioid medication may have on work duties
- Train supervisors or managers to correctly understand/implement drug policies and how to accurately assess and respond to suspected workplace opioid abuse or even overdoses
- Provide an Employee Assistance Program, which will support employees that may need treatment options or therapy when dealing with opioid addiction or dependency
- Maintain regular, thorough, and consistently updated drug testing that is current and compliant with both state laws and federal guidelines
Preventing workplace opioid abuse begins with effective training and understanding of the risks. In short, employers are encouraged to recognize that prescription drugs like opioids can have a large impact on the workplace and ignoring the problem may only make it worse. Strong enforcement policies, expanded drug testing, employee and supervisor training, and assistance programs are all important and demonstrably effective methods for employers to help prevent workplace opioid abuse.
NES Law Enforcement & First Responder Clan Lab Safety Training
NES is a leader in clandestine laboratory safety training for first responders in law enforcement, hazmat, and firefighter teams. We provide training programs and products for first responders to opioid overdoses, clandestine laboratories, marijuana grows, and other potentially hazardous sites. Learn more by visiting the NES clandestine laboratory information page.
NES provides open enrollment clan lab training on behalf of law enforcement and first responder personnel across the nation. To learn more about our clan lab training and consulting capabilities, contact us at 916-353-2360 / 1-800-NES-ADVISE (1-800-637-2384) or office@nesglobal.net.
References:
Injury Facts: Odds of Dying
National Safety Council: Poll: 75% of Employers Say Their Workplace Impacted by Opioid Use
Drugs at Work: What Employers Need to Know
How the Prescription Drug Crisis is Impacting American Employers
Mayo Clinic: How opioid addiction occurs
National Institute on Drug Abuse: Overdose Death Rates
Centers for Disease Control and Prevention: NIOSH: Opioids in the Workplace
NIOSH: Responding to a Suspected Opioid Overdose
Drug and Opioid-Involved Overdose Deaths – United States, 2013 – 2017
Using Naloxone to Reverse Opioid Overdose in the Workplace: Information for Employers and Workers
World Health Organization: Information sheet on opioid overdose
Harm Reduction Coalition: Understanding Naloxone
